Table of Contents
IV. Symptoms of psoriatic arthritis
V. Diagnosis and treatment for psoriatic arthritis
VI. Diagnosis and treatment for psoriasis
Overview
Psoriasis and psoriatic arthritis are both autoimmune disorders that can occur together. These conditions create immune responses that lead to inflammation in the body. In autoimmune diseases, the body mistakenly attacks its functions, which leads to the inflammation. This is what causes the rash in psoriasis and joint pain in psoriatic arthritis. In the case of psoriasis, medications like Soriatane can help reduce this immune response.
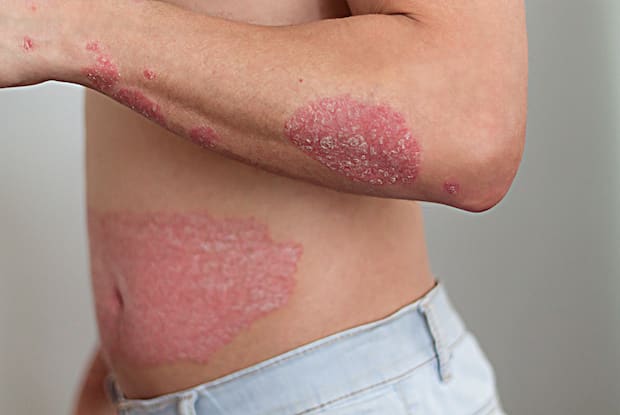
Psoriasis is a condition that causes skin cells to renew too quickly, which results in red, scaly skin patches (plaques). Psoriatic arthritis is inflammation that makes the joints feel stiff, swollen, and achy. This condition may cause long-term damage on the lower back, wrists, knees, or ankles.
Around 10 to 30 percent of those with psoriasis will develop psoriatic arthritis. The diseases are related, but they do not necessarily predict one another. Lots of people with psoriasis will never develop psoriatic arthritis, and some people will develop psoriatic arthritis without the presence of psoriasis.
What’s the connection?
Both psoriasis and psoriatic arthritis are chronic diseases that often get worse over time. Both of these diseases also have periods of remission, as well as factors that trigger flare-ups. There is no cure for either of these conditions, but there are treatments for managing symptoms.
There is no exact cause for psoriatic arthritis or psoriasis, but both occur because of malfunctions in the immune system. In the case of psoriasis, this malfunction causes the skin cells to grow too fast. With psoriatic arthritis, the inflammation affects the joints. For both conditions, the cause is typically a combination of genetic and environmental factors. Many people have the genes for a psoriatic disease but may never develop it.
The following triggers can cause psoriasis as well as psoriatic arthritis:
- An infection (strep throat or cold)
- Heavy alcohol use
- Dry indoor air
- Certain medications
- An injury to the skin
- Stress
- Cold weather
- Use of tobacco
Symptoms of psoriasis
Psoriasis is a common skin condition that speeds up the life cycle of skin cells. These extra skin cells build up rapidly to form itchy and red patches of skin. Lifestyle measures like moisturizing and managing stress can help prevent symptoms and flare-ups.
Types of psoriasis include:
Plaque psoriasis: This is the most common form that causes dry, raised, red skin lesions with silvery scales. This type can occur anywhere on the body.
Nail psoriasis: Psoriasis that affects the fingernails, which causes pitting and abnormal nail discoloration. Severe cases may cause the nail to crumble from the nailbed.
Guttate psoriasis: This type is usually triggered by a bacterial infection and causes water-drop shaped scaling lesions on the trunk, arms, legs, and scalp.
Inverse psoriasis: This type affects the skin in the groin, armpits, under the breasts, and around the genitals. Inverse psoriasis causes smooth patches of red to appear where skin rubs against itself.
Pustular psoriasis: This type is uncommon and creates pus-filled blisters on the plaques of red skin.
Erythrodermic psoriasis: This is the least common type of psoriasis, which can create a red and peeling rash that can itch intensely. This type affects those with unstable plaque psoriasis.
Each type of psoriasis can present itself differently, but some common symptoms can include:
- Red patches of skin, covered in silvery scales
- Thickened or pitted nails
- Swollen and stiff joints
- Cracked skin that may bleed [1]
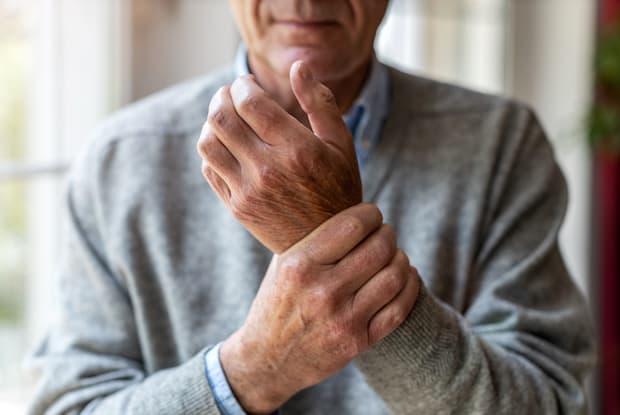
Symptoms of psoriatic arthritis
Psoriatic arthritis is a chronic inflammatory disease of the joints, especially of the places where tendons and ligaments connect to bone. This disease usually affects people between 30 and 50 years old. In some cases, psoriatic arthritis occurs around 10 years after being diagnosed with psoriasis. Psoriatic arthritis is different than other forms of arthritis, and this condition has two unique signs:
1) Enthesitis: This condition occurs when tender spots appear where the tendons and ligaments join onto the bones. These sore spots usually occur in the feet, elbows, ribs, spine, and pelvic area.
2) Dactylitis: The fingers or toes appear swollen or sausage-like. This can occur in one or multiple digits.
- More signs and symptoms of psoriatic arthritis can include:
- Fatigue
- Sore or red eyes
- Painful or sore tendons
- Spondylitis, which is the stiffness or pain in the back or neck that makes it difficult to bend or move the back
- Reduced range of motion
Early recognition and diagnosis of psoriatic arthritis is essential because permanent joint damage can occur if this condition is left untreated.
Diagnosis and treatment for psoriatic arthritis
To diagnosis psoriatic arthritis, a doctor may:
- Check your fingernails for pitting, flaking, and other abnormalities
- Examine your joints for signs of swelling or tenderness
- Press on the soles of your feet and heels to identify tender areas
Some tests may include:
X-rays: X-rays can help a doctor determine changes in the joint.
Magnetic resonance imaging (MRI): This test used radio waves and a strong magnetic field to make detailed images that can show problems in the tendons and ligaments.
Rheumatoid factor (RF): This blood test is taken to show if the RF antibody is present in the blood. The antibody is only present in those with rheumatoid arthritis but not in psoriatic arthritis.
Joint fluid test: In this test, a needle is inserted into one of your affected joints, and a small sample of fluid is taken. The test will determine if you have psoriatic arthritis or another joint illness, like gout.
Since there is no cure for this condition, treatment focuses on controlling inflammation of the affected joints. Read on for some common medications used to treat psoriatic arthritis.

Disease-modifying antirheumatic drugs (DMARDs): These drugs can slow the progression of psoriatic arthritis and could save the joints from further damage. Some common medications can include Arava and Trexall.
Biologic agents: Biologic agents are a newer class of DMARDs and can target specific parts of the immune system that cause the inflammation of the joints. These drugs should be used with doctor supervision because they can increase your risk of infections and blood clots.
Steroid injections: Injections of steroids into the joints can quickly reduce inflammation of an affected joint. If the joints become severely damaged, then the doctor may recommend joint replacement surgery. [2]
Diagnosis and treatment for psoriasis
Unlike some cases of psoriatic arthritis, the diagnosis of psoriasis is fairly straightforward. A combination of ointments and oral medications is often present in a psoriasis treatment plan.
The doctor will likely perform the following to determine your condition:
Physical exam and medical history: Psoriasis can be an inherited condition, and your doctor will discuss your medical history. They will also examine your skin, scalp, and nails.
Skin biopsy: A skin biopsy is taken in rare cases to be examined under a microscope to determine the type of psoriasis you are experiencing.
Your treatment depends on the type of psoriasis and the severity of your symptoms. Treatment methods can include:
Light therapy (Phototherapy): Light therapy uses natural or artificial ultraviolet light. Exposing the skin to controlled amounts of natural sunlight can improve the condition of the skin.
Topical treatments: Your doctor may prescribe creams or ointments to treat mild or moderate psoriasis. Topical corticosteroids can reduce redness and relieve itching. These are often used for a short time to avoid any side effects. Other topical treatments include salicylic acid, topical retinoids, and vitamin D lotions.
Oral medications: If your psoriasis is resistant to creams or light therapy, oral medications are prescribed. Vitamin A retinoids like Soriatane are used to reduce the symptoms of severe psoriasis. Methotrexate drugs and cyclosporine can suppress inflammation and the immune system to lessen symptoms. [3]
The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis or treatment.
